Essay
The W.H.O.’s pandemic treaty may spark a global health revolution
Read Part I of the series BY INDIA-BASED GLOBAL HEALTH WRITER, VIDYA KRISHNAN, on THE GLOBAL PANDEMIC RESPONSE.
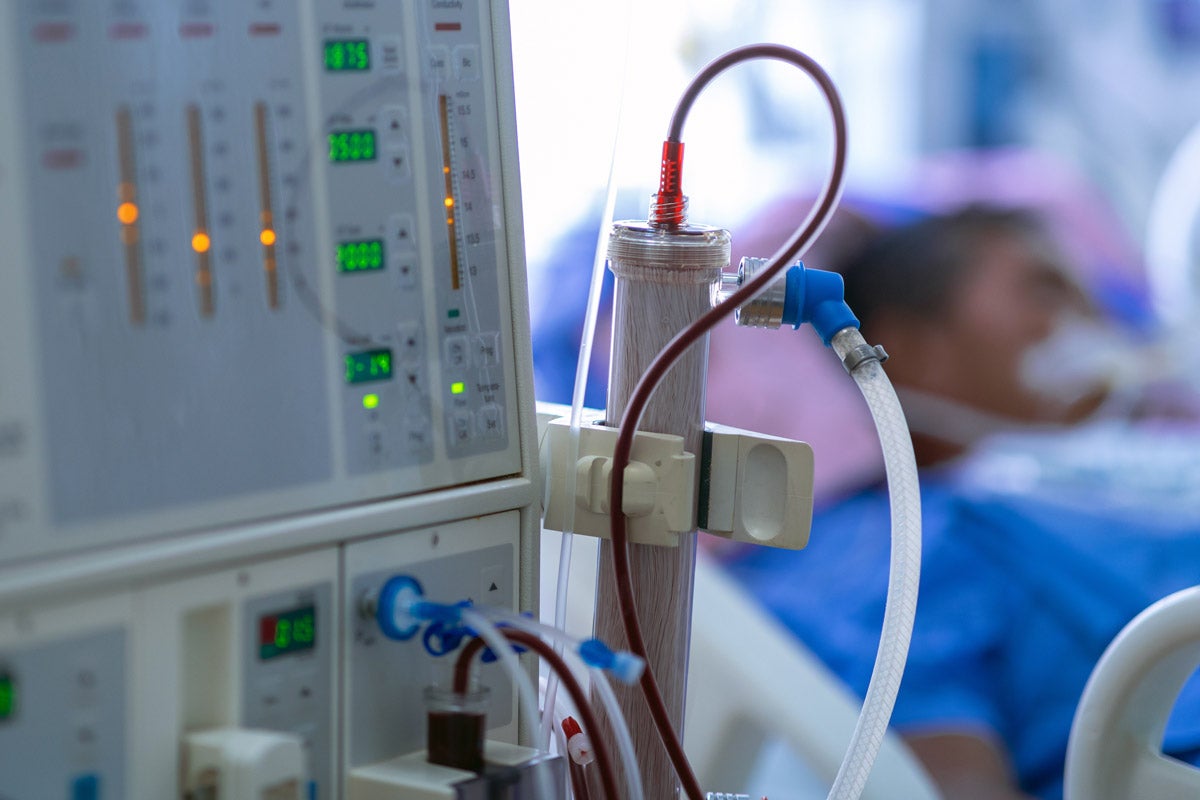
In the summer of 2021, the deadly Delta variant hit my home country of India with unchecked ferocity, swallowing an estimated 2.7 million lives in just four months.[1] A World Health Organization report from May 2022 estimates nearly 5 million Indians died from COVID-19, more than any other country.
Every country has faced its share of horrors from the coronavirus pandemic, but in India people died like the medieval wretches of 14th century Sicily suffering from the Black Death. News reports and social media posts from the darkest days of the Delta wave were macabre accounts of desperate people scrambling for scarce oxygen cylinders, hospital beds, ventilators, and ambulances—and then for coffins and wood for funeral pyres. For months, India lay prostrate, at the mercy of the plague.
What does it say about the global health system that India, a country with immense resources, some of the best doctors in the world, scientific expertise, unmatched experience in dealing with infectious diseases, and a major manufacturing hub of COVID-19 vaccines, descended into a viral apocalypse?
Sign up for Harvard Public Health
Delivered to your inbox weekly.
The problem is that a vast body of research, money, and pharmaceutical know-how has been monopolized by just a few nations like the United States, Canada, Japan, Germany, Switzerland, and the United Kingdom.
In fact, it took 20 months of negotiation to arrive at a compromise on waiving patent rights to COVID-19-related technology, as rich nations stalled and blocked discussions. The eventual agreement only covered vaccines, leaving out diagnostics and therapeutics, and only lasts for five years. By keeping vaccine supply scarce and prices high, the companies that monopolized the development and production of COVID-19 vaccines for the first two years of the pandemic—Pfizer, BioNTech, and Moderna—made combined profits of $65,000 a minute during the pandemic.
But a revolution is brewing, one in which the world is taking steps to decolonize the existing international laws governing our ongoing global health response to infectious diseases of all kinds. In October 2020, India and South Africa asked the World Trade Organization to do away with patent enforcement for all COVID-19 medicines, tests, and vaccines for the duration of the pandemic, a move they didn’t realize at the time would come to represent a watershed moment of mobilization amongst post-colonial nations. What began as an almost mundane effort to cut global health red tape became a much larger fight against the prevailing intellectual property regime. Pharmaceutical companies in rich nations fought back, but post-colonial nations haven’t wavered in their continued protest against an unjust intellectual property system, and have brought a long overdue level of public scrutiny to the development of new treatments and vaccines.
Pfizer, BioNTech, and Moderna made combined profits of $65,000 a minute during the pandemic.
In 2021, the 194 member states of the World Health Organization began negotiating a new international agreement to replace the existing International Health Regulations—a treaty governing global health emergencies adopted in 2005—and influence implementation of the Trade-Related Aspects of Intellectual Property Rights (TRIPS) agreement governed through the WTO, the global standard for intellectual property rights. The two treaties have long been at odds in times of emergency, and although TRIPS allows for the use of a patented product without permission during national or global emergencies, the COVID-19 pandemic has only underscored how reluctant rich nations are to actually share vaccines and drugs, even in emergencies. In 2021, rich nations blocked just such a TRIPS waiver that would help countries overcome legal barriers to producing their own COVID-19 vaccines and treatments (they later approved a partial TRIPS waiver). The new treaty in the works may better position the world to prevent, respond and prepare for future pandemics. On February 1, 2023, the WHO released a “zero draft” of what has come to be known simply as the “pandemic treaty.”
The treaty is an unprecedented attempt to address a blind spot in international law when it comes to global action on pandemics: information sharing—something the world failed spectacularly to do during the COVID-19 pandemic. Like all important conversations, it is many things in one, and includes a new approach to the ethics of medicine, health, and trade in times of emergency. The fact that it’s always been the WTO, not the WHO, that has governed how the world transfers scientific knowledge between countries to protect and advance health betrays a deep malignancy at the core of the world order: that it is money, not the public’s health, driving decision-making at the highest levels of international governance.
And rich countries hold most of the cards. In medical historian Alexandre White’s recent book, Epidemic Orientalism: Race, Capital, and the Governance of Infectious Disease, he notes the International Health Regulations “position Europe and more broadly the West as the sites that must be protected from the infectious disease threats of the rest of the world.”
The coronavirus pandemic was a textbook example of epidemic orientalism. As rich countries hoarded vaccines, poorer countries without manufacturing capacity were left relying on donations through COVAX—a global initiative co-led by the WHO to create equal access to vaccines. COVAX was a vision of genuine global solidarity, launched in April 2020 with one primary vaccine supplier: India, a country that has long been a bulwark of vaccine manufacturing and the pharmacy of the developing world. The viral apocalypse that hit India is partly because of its role as a vaccine manufacturer.
It is money, not the public’s health, driving decision-making at the highest levels of international governance.
In early 2021, Indian factories were pumping out millions of vaccine doses which were distributed to 95 countries via COVAX. In May 2021, around the time the Delta wave began, only four percent of India’s 1 billion people were vaccinated.[2] In the U.S., that number was upwards of 40 percent. When India stopped exporting vaccines to meet its own demands, African nations were left out in the cold. Rich countries failed to step in with their vaccine reserves to fill the gaps.
All of this underscores the need for a new paradigm. The pandemic treaty obliges pharmaceutical companies to disclose information on public funds they use for research and development, product pricing, and contract terms for public procurement during a pandemic—all common-sense measures that should apply even in non-pandemic times. The treaty is likely to be negotiated through 2024, and is the first genuine step towards decolonizing international law governing the global response to infectious disease outbreaks. The roots of the governing International Health Regulations can be traced to 19th century colonial agreements to stop the spread of infectious disease. Its legacy includes a xenophobic and racist fixation on preventing the spread of disease from Asia to Europe.
As a result, the International Health Regulations prioritize only the notification of public health emergencies without requiring countries to mobilize and share information on a range of counter-measures like diagnostics, vaccines, and therapeutics.
The new pandemic treaty on the other hand is a departure from the earlier model. The British Medical Journal in a recent editorial noted, “in the draft treaty, pathogen access and benefit sharing would apply in pandemics and in between them, with the intent of establishing a multilateral, fair, equitable, and timely system for accessing pathogens with pandemic potential and their genomic sequences and for the equitable sharing of benefits that arise from their use. This includes real time access by the WHO to 20% of pandemic-related product volumes, such as vaccines, distributed on the basis of public health risk and needs, especially to developing countries.”
When the next pandemic washes ashore, the best solution is to make sure each continent has the capacity to manufacture and supply its own needs without being left to the charity of wealthy nations. The new pandemic treaty, if adopted, may help prevent future pandemics from wreaking havoc in low-income countries, and accelerate new treatments and vaccines for existing ones like tuberculosis.
People of the Global South are organizing to change the global health order. The pandemic years have seen unprecedented R&D funding for African nations, and increased vaccine manufacturing capacity, including for mRNA vaccines. Other important lessons have been learned, too. India now knows it cannot be the only pharmacy for the developing world in a pandemic. The new reality is that a global response cannot be built around donations, charity, or the largesse of billionaires.
The fire of revolution has been lit. And fortunately for us, like plagues, radical ideas are infectious, too.
Source images: Jason Leung/ Unsplash, dangrytsku / iStock
[1] The Indian government has reported 530,771 COVID-19 deaths as of January 31, 2023. Experts argue the true count may exceed 3 million.
[2] An estimated 80 percent are now fully vaccinated as of the end of 2022.