Opinion
Empathy should guide responses to reported vaccine injuries
This essay was originally published by STAT on June 11, 2024.
As a coleader of the team at the National Institutes of Health that developed technologies powering a number of COVID-19 vaccines, I often speak publicly about vaccine science, even though I no longer work for the government. After my talks, people often approach me, almost always thanking me for my work. There is no denying the millions of lives that COVID-19 vaccines saved. Sometimes, though, they relate stories of vaccine injuries.
I still hold on to the story of one person who approached me in a crowded auditorium following one of my talks, asserting that the COVID-19 vaccine harmed her. She asked me what I was doing to investigate vaccine injury. I replied that the side effects of vaccines, as they emerge in clinical trials, are investigated, and there is continuous monitoring of vaccinated people by the Food and Drug Administration and the federal Centers for Disease Control and Prevention.
But I wonder: Is that enough? Has my own science contributed to ignoring people who feel they have been harmed and not heard? In that moment, did I really hear this woman, who believed a COVID-19 vaccine had harmed her?
Sign up for Harvard Public Health
Delivered to your inbox weekly.
There has been increased attention on people who report long-term negative effects of COVID-19 vaccines. They are not conspiracy theorists or vaccine skeptics. They are, among others, scientists who appreciate the enormous value of vaccines.
For some of them, tinnitus—often reported as a ringing in the ears—is common. This feels like a perfect metaphor for me: Scientists ought to be better listeners, hearing people out and taking seriously personal stories of potentially vaccine-related harm. People who speak out about how they feel after getting a vaccine should not be dismissed or assumed to be anti-vaxxers.
For starters, they deserve empathy from their doctors and other health care providers, as well as from those who set and drive vaccine policy. Science owes them—and ultimately all of us—far more investment in research to validate or invalidate claims of vaccine-related harm. They must be fully investigated to prevent further vaccine-related injuries.
The COVID-19 vaccine is not the only shot for which injuries have been reported. Flu vaccines, which are updated every year, have also been linked to tinnitus and other vaccine side effects. But they generate only a small fraction of the controversy that COVID-19 vaccines did, and the rare injuries do not receive feature news coverage, though that doesn’t mean they are any less important for people who are experiencing them.
Vaccine injuries—long-term medical consequences from a shot—are real phenomena worthy of investigation. When someone somewhere feels harmed, it is the duty of scientists and health care providers to heed these people and listen. Scientists need to better understand what happened and why, so that the next iteration of a vaccine can be better. But scientists aren’t trained to appreciate anecdotes.
People who feel they have been harmed by a vaccine do not need to have the science immediately explained to them. What they first need is to be heard, and then assured that science will follow.
This kind of work should be similar to research on rare diseases: Find the relatively small number of people who have a specific reaction to a vaccine, then understand what happened and why. But until that point is reached, it is essential to lead with an explanation that is fair and correct on how the probability of experiencing the side effect was far lower than the probability of getting severely ill from COVID-19 or any other vaccine-preventable illness.
For people reporting adverse effects from vaccines, scientists and others can do better at being compassionate, starting with: We hear you. There may be no way today to prove cause and effect with your particular vaccine injury. But we fully appreciate and empathize with what you are going through and owe you and the rest of the public more information about the relationship between the vaccine and the injury you experienced.
And then there are steps that I and others in the vaccine field—everyone from researchers to vaccine regulators—should take to:
- Create a better system for reporting and investigating cases of vaccine injury to better capture and understand these experiences. These data should be consistently mined and investigated while acknowledging and respecting the people who provide their information. Examining their claims of vaccine injury can be scientifically challenging, but it is medically important.
- Develop a systematic approach to understanding potential rare vaccine side effects.
- Provide funding to support thorough investigations of vaccine-related injuries.
- Write a better playbook—with better distribution—for health care providers on how to speak with and care for people who experience vaccine-related injuries.
There is a very low probability that I will ever again see the woman who told me about her vaccine injury. Although others may follow, her impact on me has been profound. I know that she represents thousands of other people in pain, and I and other vaccine scientists owe them all a good listen and advocacy on their behalf to learn more.
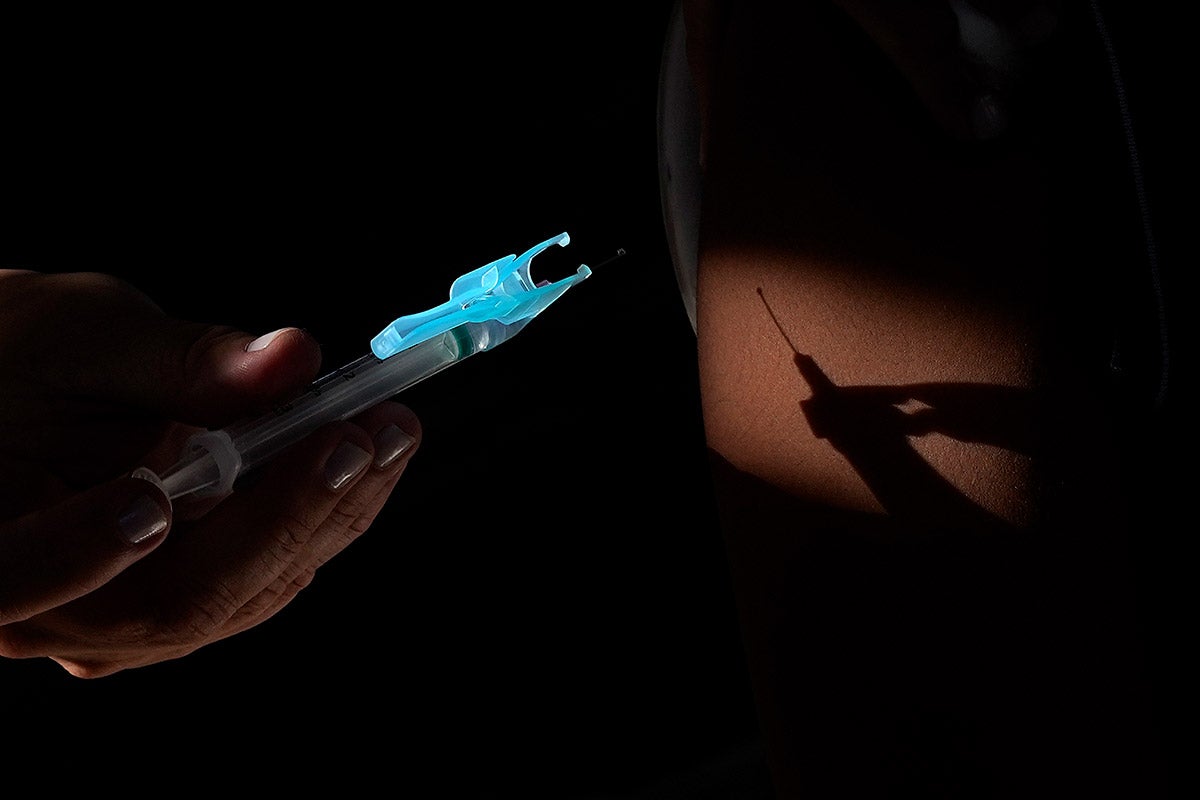
Lead image: A health worker applies a shot of the Pfizer COVID-19 vaccine at a community health center in Brasilia, Brazil, in 2022. (AP Photo / Eraldo Peres)



