School news
Frontlines Spring 2021
Kizzmekia Corbett was a leader at the NIH in the development of the COVID-19 vaccine deployed by Moderna.

Kizzmekia Corbett, assistant professor of immunology and infectious diseases
Photo: Marlayna Demond / UMBC
Kizzmekia S. Corbett will join the Department of Immunology and Infectious Diseases at the Harvard T.H. Chan School of Public Health in June as an assistant professor. She was one of the leading scientists at the National Institutes of Health (NIH) behind the development of a COVID-19 vaccine now in use throughout the world. At the Harvard Chan School, she will continue her work on coronavirus vaccine development and pursue strategies for overcoming vaccine hesitancy and addressing health disparities.
“I’m excited to join the faculty at the Harvard Chan School,” Corbett said. “This is an institution that values scientific discovery and teaching and putting in the work to translate and communicate the science to the community. I look forward to continuing to tackle big biomedical problems to improve the health of the world.”
Sign up for Harvard Public Health
Delivered to your inbox weekly.
As a research fellow at NIH and the scientific lead for coronavirus research in the Viral Pathogenesis Laboratory of the National Institute of Allergy and Infectious Diseases (NIAID) Vaccine Research Center, Corbett helped design the mRNA-1273 vaccine candidate, led the preclinical studies, and designed assays used for evaluating samples from vaccinated clinical trial participants.
Prior to the pandemic, Corbett and her colleagues worked on vaccines for other coronaviruses using mRNA technology, which delivers a piece of genetic code directly to the cells to stimulate an immune response. She also has worked on a universal influenza vaccine candidate and, over the past 19 years, studied dengue virus and respiratory syncytial virus.
Corbett holds a BS in biological sciences, with a secondary major in sociology, from the University of Maryland, Baltimore County, where she was a Meyerhoff Scholar and an NIH undergraduate scholar. She earned a PhD in microbiology and immunology from the University of North Carolina at Chapel Hill.
In February 2021, Time selected Corbett for its “Time100 Next” list under the category of Innovators and published a profile of her written by Anthony S. Fauci, director of NIAID.
Corbett is passionate about tackling health inequities and communicating science to the general public. She has been particularly focused on discussing COVID-19 science with communities of color to address concerns about the vaccine.
“Kizzmekia is a scientific leader in the way that we aspire to build scientific leaders,” said Sarah Fortune, John LaPorte Given Professor of Immunology and Infectious Diseases and chair of the Department of Immunology and Infectious Diseases. “I think that she will electrify our students and expand our sense of the possibilities of public health.”
Secret shoppers raise concerns about addiction-treatment programs

An audit of more than 600 residential care programs for opioid-use disorder raised concerns about the programs’ high costs and misleading recruitment practices, according to Harvard Chan School research published in February in Health Affairs. The secret shopper–style study had callers pose as uninsured cash-paying individuals using heroin and seeking addiction treatment. Many of the programs required up-front payments, and there was a sharp disparity in costs between for-profit and nonprofit programs, according to the study. One-third of the callers were offered admission before clinical evaluation. Corresponding author Michael Barnett, assistant professor of health policy and management, called for better regulation of residential addiction-treatment programs in an interview with WBUR in February. He said, “If a hospital was admitting anyone who walked into the emergency room regardless of how sick they are, giving them treatment that may or may not help them, we’d find that absurd.” Read more
In the liver, a stressed cell can be bad news for its neighbors

A key protein in the communication channels between cells can allow a stress response in one liver cell to spread to neighboring liver cells in mice, causing otherwise healthy cells to become dysfunctional, according to research co-led by the Harvard Chan School and Sheba Medical Center in Israel. Published in Cell Metabolism in December 2020, the study is the first to demonstrate that the protein Cx43 plays a role in the spread of endoplasmic reticulum (ER) stress signals among liver cells. After experiments on mice determined that diet-induced obesity resulted in ER stress that in turn increased levels and activity of Cx43, the team then created a line of mice lacking the protein in their liver cells. In these mice, a high-fat diet did not trigger ER stress in liver cells, and the animals were protected from insulin resistance, glucose intolerance, and nonalcoholic fatty liver disease—opening a potential pathway for prevention and treatment of a range of metabolic diseases. Read more
New links between diet and cancer risk
Eating more fruits and vegetables may help breast cancer survivors live longer, according to research led by Maryam Farvid, a former research scientist in the Department of Epidemiology. The study, published in November 2020 in Cancer Research, found that women with breast cancer who consumed higher amounts of fruits and vegetables after their diagnosis were less likely to die during the study period than those with lower amounts of fruits and vegetables in their diets. Read more
In addition, dietary patterns that are associated with inflammation and insulinemia—a condition marked by high levels of insulin in the blood—may put men at an increased risk for aggressive forms of prostate cancer, according to a separate study published in European Urology, led by postdoctoral fellow Benjamin Fu. These dietary patterns tend to be high in processed meats, sugary sweets, and fried foods and low in leafy vegetables. Read more
Most pregnant women and mothers would get COVID-19 vaccine
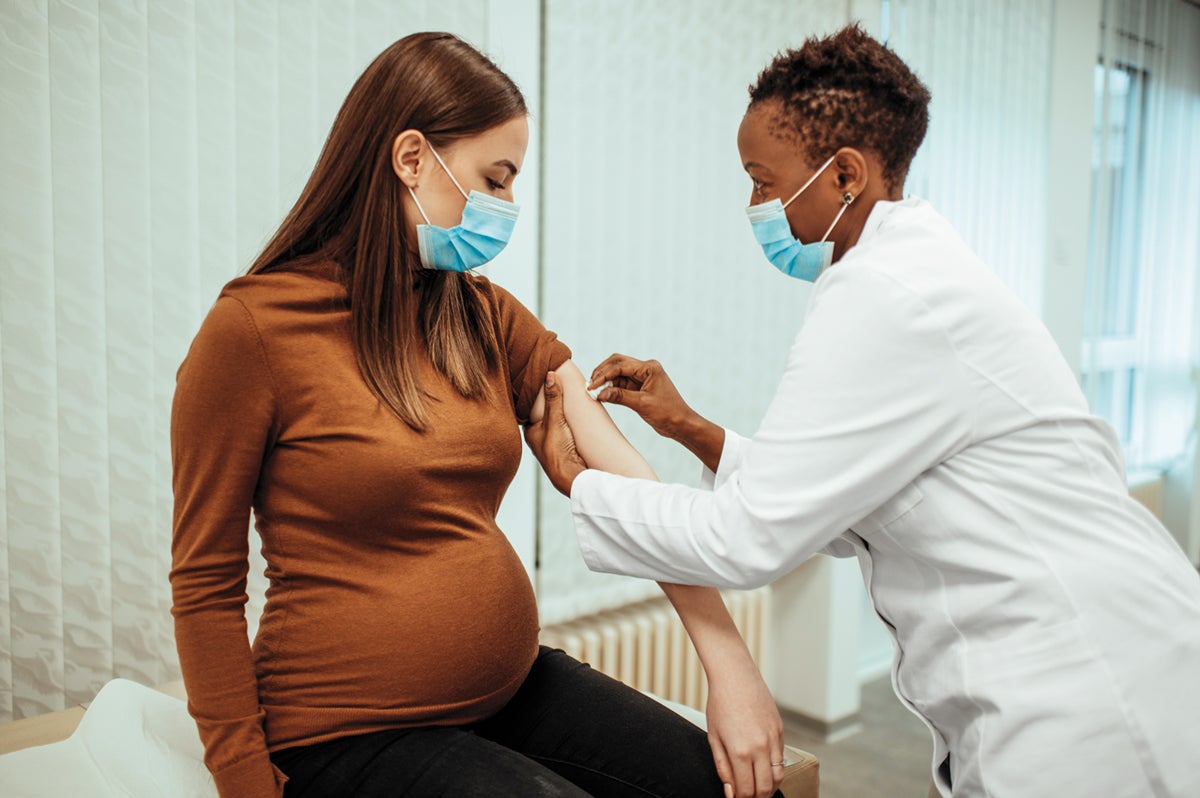
Most pregnant women and mothers of children younger than 18 years old say they would receive a COVID-19 vaccine and vaccinate their children, according to a survey conducted by researchers at the Harvard Chan School. The results indicated that vaccine acceptance was highest in India, the Philippines, and all sampled countries in Latin America, and it was lowest in Russia, the U.S., and Australia. The study was published March 1 in the European Journal of Epidemiology.
Some of the strongest predictors of COVID-19 vaccine acceptance among the women surveyed included confidence in its safety or effectiveness, worry about COVID-19, and trust in public health agencies and health sciences, said senior author Julia Wu, research scientist in the Department of Epidemiology and a principal investigator at the Human Immunomics Initiative. Read more
Donald Hopkins Scholars Lecture launches

Donald Hopkins, MPH ’70, gave the inaugural lecture in a series named in his honor in a virtual presentation on February 25.
Hopkins, special adviser for Guinea worm eradication at the Carter Center, spoke about his 40-year campaign against this painful and debilitating disease—one of public health’s great success stories. In the 1980s, there were millions of cases of Guinea worm disease across the globe, mostly in rural Africa. In 2020, there were only 27 cases worldwide.
The new lecture series is designed to highlight the research and accomplishments of scholars and educators in global and national public health. The School also hosts the Donald Hopkins Predoctoral Scholars Program, housed in the Office of Diversity and Inclusion, which offers accepted students the opportunity to study at the master’s level in anticipation of further study toward a doctoral degree. Read more
HPV vaccines for adults over age 26 may not be cost-effective
Vaccinating adults over age 26 against the human papillomavirus (HPV)—the virus that causes most cervical cancers, as well as several other cancers—may not be cost-effective, according to a new study published March 11 in PLOS Medicine.
Current U.S. guidelines recommend HPV vaccination for girls and boys at age 11 or 12 and catch-up vaccination for people through age 26 if they were not vaccinated when younger. The new study was undertaken to inform guidelines for adults over 26.
Jane Kim, dean for academic affairs and K.T. Li Professor of Health Economics, who was lead author of the study, noted that current HPV vaccines are most effective when given prior to HPV exposure, which can happen soon after sexual initiation; once someone is exposed to HPV, the vaccine won’t clear those infections. Therefore, it is likely to be of little benefit to people in their 30s and 40s.
Kim added, “It’s also important to emphasize that cervical cancer screening remains an effective and cost-effective way to protect women from cervical cancer.” Read more



